surgical tech instruments study guide
This comprehensive guide aids surgical technologists in mastering instrument identification, usage, and care, utilizing resources like pocket guides and flashcards for exam preparation.
Surgical instrumentation represents the foundational tools of the operating room, demanding precise recognition and understanding from surgical technologists. A robust knowledge base encompasses over 160 commonly utilized instruments, each serving a distinct purpose within surgical procedures.

This field requires familiarity with variations in instrument design and alternative names, ensuring seamless communication and efficient workflow. Mastering these tools isn’t merely about identification; it’s about comprehending their strategic application in diverse surgical scenarios – general surgery, laparoscopic procedures, obstetrics, gynecology, and orthopedics.
Effective instrument handling builds surgical judgment and confidence, crucial for optimal patient outcomes and a safe operating environment. Resources like illustrated flashcards and pocket guides are invaluable for this learning process.
Importance of Instrument Recognition
Accurate instrument recognition is paramount for surgical technologists, directly impacting patient safety and surgical efficiency. Misidentification can lead to procedural delays, incorrect tissue handling, and potentially adverse events. A swift and confident ability to name and understand the function of each instrument is therefore non-negotiable.
This skill fosters effective communication within the surgical team, minimizing misunderstandings during critical moments. Furthermore, recognizing instrument variations and alternative names ensures adaptability and preparedness for diverse surgical settings.
Proficiency in instrument identification is a core competency assessed in technologist exams, emphasizing its fundamental importance in the field.
Basic Instrument Classification
Surgical instruments are broadly categorized by their primary function, streamlining organization and facilitating efficient case setup. These classifications include cutting & dissecting tools – scalpels, scissors, and specialized devices for precise tissue manipulation. Grasping & holding instruments, like forceps and needle holders, secure tissues for visibility and control.

Retracting instruments maintain surgical field exposure, while hemostatic tools – clamps – control bleeding. Suturing instruments, encompassing needles and materials, enable wound closure.
Additionally, specialty sets cater to specific procedures, such as laparoscopic, OB/GYN, and orthopedic surgeries, each containing tailored instrumentations.
Cutting & Dissecting Instruments
This category encompasses tools designed for precise tissue separation and resection. Scalpels, with their interchangeable blades, offer varying shapes and sizes for diverse incisions. Scissors, available in numerous types – Mayo, Metzenbaum, and others – facilitate tissue dissection and cutting with differing precision.
Specialized cutting tools, like rasps and osteotomes, address specific surgical needs, such as bone shaping. Understanding the nuances of each instrument – blade types, scissor curvature, and tool-specific applications – is crucial for effective surgical assistance.
Scalpels and Blades
Scalpels are fundamental cutting instruments, consisting of a handle and detachable blades. Blade selection is paramount, dictated by incision depth and tissue type. Common blade shapes include #10, #11, #15, and #20, each designed for specific surgical tasks. Handles come in various styles – disposable, reusable – influencing grip and control.
Technologists must master blade changing techniques, ensuring secure attachment and safe disposal. Understanding blade numbering systems and their corresponding applications is vital. Proper handling minimizes risk and optimizes surgical precision, contributing to successful outcomes during procedures.
Scissors: Types and Uses
Surgical scissors are diverse, categorized by structure and function. Mayo scissors, robust with blunt tips, dissect heavy tissues. Metzenbaum scissors, delicate with sharp points, are ideal for fine dissections. Iris scissors excel in precise cuts during ophthalmic procedures. Stitch scissors feature a snip for suture removal.
Technologists must differentiate these types, understanding their specific applications. Recognizing variations – straight, curved, angled – is crucial for anticipating the surgeon’s needs. Proper handling ensures clean cuts and minimizes tissue trauma. Maintaining sharpness through regular inspection is essential for optimal performance.
Specialized Cutting Tools
Beyond scalpels and scissors, surgical teams utilize specialized cutting instruments for specific tasks. Bone cutters, like the Gigli saw, precisely transect bone tissue. Curettes, spoon-shaped tools, scrape tissue for biopsies or removal. Rotary burrs, attached to power equipment, shape and smooth bone surfaces.
Understanding these tools requires recognizing their unique mechanisms and appropriate applications. Technologists must anticipate the surgeon’s needs, ensuring the correct instrument is available. Safe handling is paramount, given the potential for injury. Proper maintenance, including blade replacement and sterilization, guarantees optimal function and patient safety.
Grasping & Holding Instruments
Grasping and holding instruments are fundamental to surgical procedures, enabling precise tissue manipulation; Forceps, available in numerous variations, securely grip tissues for dissection, retraction, or hemostasis. Needle holders, notably the Mayo-Hegar, firmly grasp suture needles for controlled passage through tissue. These instruments demand a thorough understanding of their mechanics.
Technologists must differentiate between various forceps types – tissue, hemostatic, and dissecting – based on their jaw design. Proper instrument handling prevents tissue damage. Anticipating the surgeon’s needs and providing the correct grasping tool streamlines the operation and enhances surgical precision.
Forceps: Variations and Applications
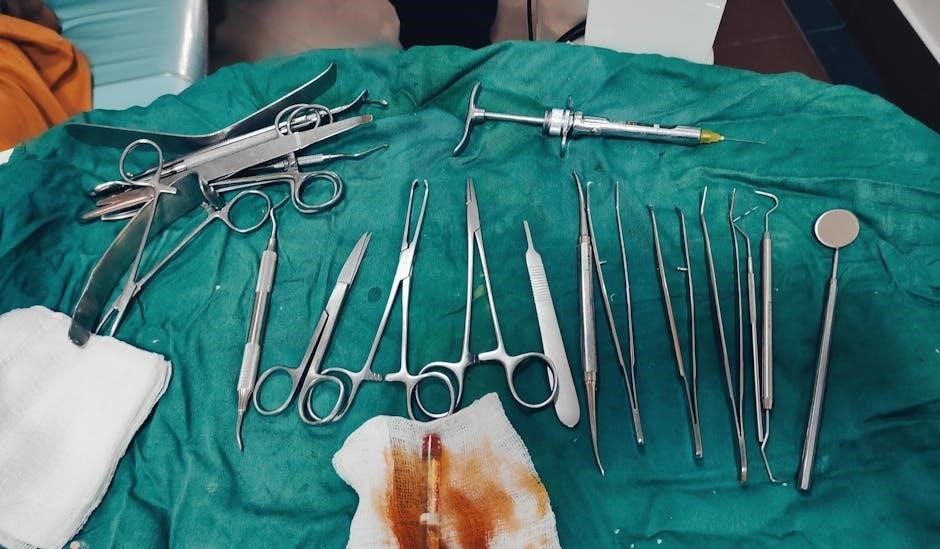
Surgical forceps exhibit diverse designs tailored for specific tasks. Tissue forceps, like Adson and DeBakey, gently grasp delicate tissues, minimizing trauma. Hemostatic forceps – Kelly, Mosquito, and Crile – clamp vessels to control bleeding. Ratcheted and non-ratcheted options offer varying grip strengths. Serrated or smooth jaws impact tissue damage potential.
Applications range from grasping skin edges during closure to manipulating intestines during resection. Technologists must recognize each type and anticipate the surgeon’s needs. Proper selection and handling are crucial for optimal surgical outcomes, preventing tissue compromise and ensuring efficient procedures.
Needle Holders: Mayo-Hegar and Others
Mayo-Hegar needle holders are fundamental suturing tools, adaptable across general surgery; These instruments securely grasp needles for precise tissue approximation. Variations include different jaw designs – smooth, textured, or with multiple teeth – influencing grip strength. Other types, like Castroviejo, offer specialized features for delicate microsurgery.
Technologists must understand how to load, lock, and unlock needles correctly. Proper technique prevents needle bending or slippage during suture placement. Recognizing the surgeon’s preference and the specific surgical context dictates the appropriate needle holder selection, ensuring efficient and accurate wound closure.
Tissue Forceps: Identifying Different Types
Tissue forceps are crucial for grasping and manipulating tissues during surgery. Numerous types exist, each designed for specific applications. Adson forceps feature fine teeth for delicate tissue handling, while Debakey forceps offer atraumatic grasping with minimal tissue damage. Russian forceps boast interdental ridges for firm grip on dense tissues.
Identifying forceps by their shape, tooth pattern, and size is essential. Technologists must understand which forceps are appropriate for different tissue types and surgical procedures. Proper handling prevents tissue trauma and ensures optimal surgical field visualization, contributing to successful outcomes.
Retracting Instruments
Retracting instruments are vital for exposing the surgical site, providing clear visualization for the surgeon. These tools hold tissues and organs out of the way, creating and maintaining surgical access. Retractors are broadly categorized as handheld or self-retaining.
Handheld retractors, like Army-Navy and Richardson retractors, require a surgical assistant to maintain tension. Self-retaining retractors, such as Weitlaner and Balfour retractors, lock into place, freeing the assistant. Understanding the different types and their appropriate applications is crucial for efficient surgical workflow and optimal patient outcomes.
Handheld Retractors
Handheld retractors demand a dedicated surgical assistant to apply and maintain the necessary retraction force. Common examples include the Army-Navy, Richardson, and Senn retractors, each designed for specific anatomical locations and tissue types. The Army-Navy retractor features a double-ended design for versatile use, while Richardson retractors offer various blade shapes and sizes.
Effective use requires precise positioning and consistent pressure to avoid tissue trauma. Assistants must anticipate the surgeon’s needs, smoothly adjusting the retractors throughout the procedure. Proper technique ensures optimal surgical field exposure without compromising patient safety or surgical precision;
Self-Retaining Retractors
Self-retaining retractors mechanically hold tissues apart, freeing the surgical team’s hands for other tasks. These instruments feature a ratcheting mechanism or interlocking blades to maintain retraction without constant manual pressure. Common types include the Balfour, Weitlaner, and Gelpi retractors, each suited for different surgical approaches.
Balfour retractors are frequently used in abdominal procedures, while Weitlaner retractors excel in superficial wound management. Gelpi retractors provide deep retraction in thoracic or major vascular surgeries. Careful selection and proper application are crucial to prevent tissue damage and ensure adequate surgical visualization.
Hemostatic Instruments
Hemostatic instruments are vital for controlling bleeding during surgical procedures. This category encompasses clamps – like Kelly, Mosquito, and Crile – used to occlude blood vessels. Kelly clamps are general purpose, Mosquito clamps are smaller for delicate vessels, and Crile clamps offer stronger gripping power.
Understanding suture ligatures and knot-tying techniques is also crucial for hemostasis. Ligatures provide permanent vessel occlusion, while secure knots ensure lasting control. Proper instrument handling and knowledge of vascular anatomy are essential for effective hemostasis, minimizing blood loss and improving surgical outcomes.
Clamps: Kelly, Mosquito, and Crile
Surgical clamps are essential hemostatic devices, each designed for specific vascular control needs. Kelly clamps, with their interlocking teeth, provide a secure grip on larger vessels and tissues. Mosquito clamps, smaller and more delicate, are ideal for clamping smaller vessels with minimal trauma.
Crile clamps, distinguished by their curved shape and strong clamping force, are frequently used in deeper surgical fields. Technologists must recognize the subtle differences in design and application to ensure appropriate instrument selection, contributing to effective hemostasis and optimal surgical field visualization.
Suture Ligatures and Knots
Suture ligatures secure tissues together, demanding a thorough understanding of knot-tying techniques. Surgical technologists must anticipate the surgeon’s needs, preparing appropriate suture materials and assisting with knot placement. Mastering various knot types – square, surgeon’s, and instrument ties – is crucial for wound closure.
Proper tension and security are paramount; a poorly tied knot can compromise tissue approximation. Understanding the principles of knot security, including throw count and knot placement, directly impacts patient outcomes. Accurate anticipation and efficient assistance with suturing are hallmarks of a skilled surgical technologist.
Suturing Instruments
Suturing instruments are essential for wound closure, with needle holders like the Mayo-Hegar being particularly versatile in general surgery. Technologists must recognize diverse needle types – curved, straight, and specialized – understanding their characteristics and appropriate tissue applications.
Furthermore, knowledge of suture materials is critical; absorbable sutures are broken down by the body, while non-absorbable sutures require removal. Selecting the correct suture material based on tissue type and desired healing time is a key responsibility. Proficiency with these instruments and materials ensures optimal surgical outcomes and patient care.
Needle Types and Characteristics
Surgical needles exhibit diverse designs, categorized by shape – commonly curved or straight – and point style, influencing tissue penetration. Curved needles facilitate suturing in confined spaces, while straight needles are suited for superficial closures. Needle characteristics include gauge (diameter), length, and the presence of an eye (swaged or atraumatic).
Atraumatic needles, with the suture embedded within, minimize tissue trauma. Understanding these features is crucial for selecting the appropriate needle for specific surgical procedures and tissue types, ensuring precise and efficient wound approximation.
Suture Materials: Absorbable vs. Non-Absorbable
Suture selection hinges on whether absorption is desired. Absorbable sutures, broken down by hydrolysis or enzymatic action, are ideal for internal tissues where long-term support isn’t needed – examples include polyglactin 910 and chromic gut. Non-absorbable sutures, like silk or polypropylene, remain intact, suitable for skin closure or areas requiring prolonged tensile strength.
Factors influencing choice include tissue type, patient factors, and the surgical procedure. Understanding the properties of each material is vital for optimal wound healing and minimizing complications.
Specialty Instrument Sets
Surgical specialties necessitate unique instrument sets. Laparoscopic sets feature specialized trocars, graspers, and cameras for minimally invasive procedures. OB/GYN sets include instruments for deliveries, hysteroscopies, and gynecological surgeries, like forceps and curettes. Orthopedic sets contain saws, drills, and retractors designed for bone manipulation and joint reconstruction.
Technologists must recognize these sets, understand their specific components, and ensure proper setup for each surgical case. Familiarity with these specialized tools is crucial for efficient and safe surgical workflows.
Laparoscopic Instruments
Laparoscopic surgery utilizes specialized instruments for minimally invasive procedures. These sets include trocars for port access, graspers for tissue manipulation, and specialized scissors for precise dissection. Cameras and light sources provide visualization within the abdominal cavity. Instruments are often elongated and angled to navigate within the confined surgical space.
Technologists must understand the function of each component and ensure proper setup and maintenance. Recognizing variations in grasper tips and trocar sizes is essential for assisting the surgical team effectively during laparoscopic cases.
OB/GYN Instruments
Obstetric and gynecological surgery requires a unique instrument array. Sets include uterine clamps, tenacula for manipulating the cervix, and various curettes for endometrial procedures. Needle holders, specifically Mayo-Hegar, are frequently used for suturing during episiotomies or cesarean sections. Specialized retractors, like the DeLee retractor, aid in delivery.
Technologists must be proficient in recognizing these instruments and anticipating the surgeon’s needs during deliveries, hysterectomies, and other OB/GYN procedures. Proper instrument counting is crucial in this patient population.
Orthopedic Instruments
Orthopedic procedures demand specialized instruments for bone and joint manipulation. These sets commonly feature bone saws, osteotomes for shaping bone, and various types of drills and reamers. Reduction forceps are essential for aligning fractured bones, while internal fixation devices like plates, screws, and rods require specific applicators.
Knowledge of these instruments, alongside proficiency in retractors for surgical site exposure, is vital. Technologists must understand the nuances of each tool to support successful fracture repair, joint replacement, and arthroscopic surgeries.
Instrument Care and Maintenance
Maintaining surgical instruments is paramount for patient safety and longevity of the tools. Proper cleaning, sterilization, and inspection are crucial steps. Sterilization procedures, often utilizing autoclaves, must adhere to strict protocols to eliminate microorganisms.
Furthermore, meticulous instrument counting before, during, and after procedures ensures accountability and prevents retained surgical items. Regular maintenance, including lubrication and sharpening, prevents damage. Technologists play a vital role in upholding these standards, contributing to a sterile and efficient operating room environment.
Sterilization Procedures
Effective sterilization is the cornerstone of infection control in surgery. Common methods include steam sterilization (autoclaving), utilizing high pressure and temperature to kill all microorganisms. Other techniques, like chemical sterilization with solutions such as hydrogen peroxide, are employed for heat-sensitive instruments.
Rigorous adherence to established protocols, including proper packaging, loading, and cycle monitoring, is essential. Biological indicators, such as spore tests, verify sterilization effectiveness. Documentation of each cycle is critical for quality assurance and regulatory compliance, ensuring a safe environment for both patients and staff.
Instrument Counting and Accountability
Meticulous instrument counting is paramount to patient safety, preventing retained surgical items. This process occurs three times: before, during, and after surgery. The surgical team, including the scrub tech and circulating nurse, collaborates to verify instrument, sponge, and needle counts.

Any discrepancies must be immediately investigated and resolved before wound closure. Detailed documentation of counts is crucial. Accountability extends to instrument tracking systems, ensuring each instrument is accounted for throughout the surgical process, minimizing risk and upholding standards of care.
Resources for Further Study
Expanding your knowledge beyond core curriculum is vital. “Surgical Instruments: A Pocket Guide” (9781437722499) offers a quick reference for over 160 instruments, complete with photos and usage details. CSTSetup provides handy guides on instrument selection and application, enhancing surgical judgment.
“Surgical Instrumentation Flash Cards” (9780803628977) are excellent for exam preparation, covering general, laparoscopic, OB/GYN, and robotic surgery. Online resources and continuing education courses further refine skills, ensuring competency and staying current with evolving surgical technologies and best practices.











Leave a Comment